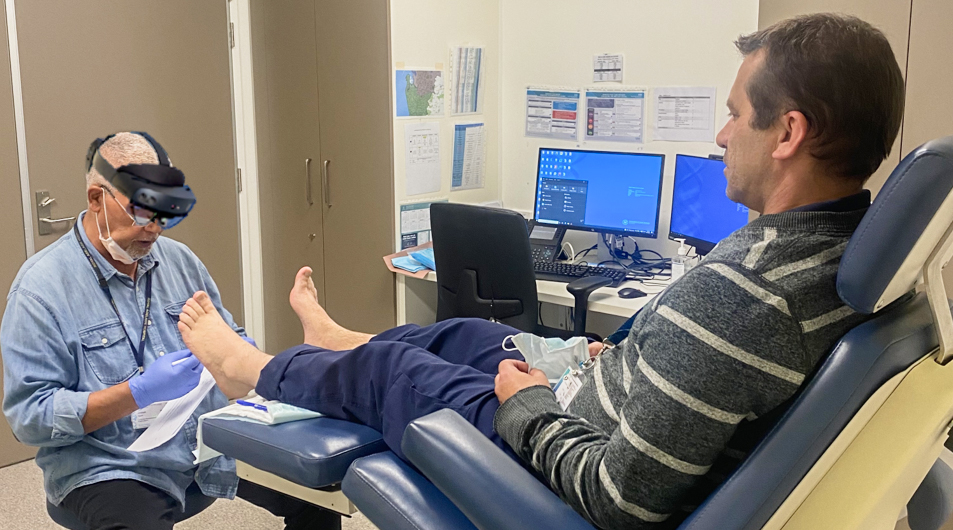
Patients in regional and remote areas could get better access to specialist care in the future thanks to mixed-reality smart glasses with holographic features.
Researchers from Central Adelaide and The University of Adelaide are developing new software that will allow specialists working in the city to “see through the eyes” of rural health workers in real time as they assess and treat patients’ leg and foot ulcers.
Specialist care in local hands
Diabetes-related foot disease is a rising problem, and particularly affects rural and remote Australians who have less access to specialist care, according to Dr Neil McMillan, Principal Medical Scientist at The Basil Hetzel Institute, The Queen Elizabeth Hospital.
“Reduced access to health services outside of the city contributes to delayed screening and detection of disease in rural communities, not to mention the financial burden on patients and the health system,” said Dr McMillan.
The software will allow remote health workers to have their hands free for performing necessary procedures such as treating wounds and changing dressings under the direction of a specialist.
“This new technology will potentially change how wounds are treated, and the way telemedicine is practiced,” said Dr McMillan.
The study, lead by Professor Rob Fitridge, Vascular and Endovascular Surgeon at the Royal Adelaide Hospital and The Queen Elizabeth Hospital, could particularly benefit Aboriginal and Torres Strait Islander consumers, who are 38 times more likely to undergo amputations associated with diabetes
“We will be able to help train local Aboriginal and non-Aboriginal health workers to assess and treat lower-limb complications using our included mixed-reality education package, which has been specifically designed for cultural safety and relevance to Aboriginal communities,” he said.
The project is a collaboration including the University of Adelaide, Insight Via Artificial Intelligence, SA Health, and UniSA, and has received $2.27 million over four years from the Medical Research Future Fund’s National Critical Research Infrastructure Scheme.