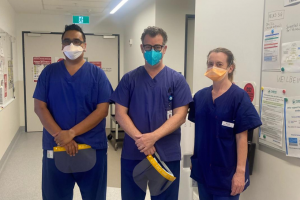
Central Adelaide’s ICU nurses are sharing their expertise with colleagues across the state as other hospitals start to care for COVID-positive patients.
Teams from the local health networks meet virtually every fortnight to discuss experiences, policies and procedures to help with planning and response efforts.
ICU acting nurse unit manager Andre, who has worked at the RAH for 17 years, says they believe information and knowledge should be shared.
“It’s really important to provide other intensive care units and networks with the opportunity to ask questions and to learn from our experience about what works and what doesn’t.
“We’re a large and well-resourced intensive care unit at the RAH and we want to help others who may have smaller intensive care teams or units. These units may need to do patient retrievals, or deal with outbreaks and/or need advice on how to set up medical emergency response services.”
Ahead of the borders opening in South Australia, the Central Adelaide ICU team were in touch with their counterparts in Melbourne and Sydney hospitals to find out what they were doing in their care of COVID-positive patients.
This, Andre says, really helped them to prepare and to know what to expect.
At the RAH itself, the ICU team have upskilled staff from other areas to become our surge workforce and step in to help the COVID ICU response. These staff were trained in basic ventilation and various modes of delivering oxygen, including nasal high flow.
“We’ve also done work around assessment skills to help staff recognise and respond to clinical deterioration in accordance with the national standard,” Andre says.
A COVID positive patient may have to go into ICU for close monitoring if they’ve deteriorated and there are respiratory issues requiring a higher level of care.
As a quaternary service, the ICU team at the RAH can provide all the different levels of treatment for COVID, including extracorporeal membrane oxygenation (ECMO) if required.
This is when blood is pumped outside of the body to a heart-lung machine that removes carbon dioxide and sends oxygen-filled blood back to the tissues in the body.
In the case of COIVD, this method allows the blood to “bypass” the lungs, allowing them to rest and heal. Luckily, we have not yet had to use this high-risk therapy.
Andre says the patients they are seeing in ICU under this Omicron wave are presenting differently.
“With previous strains, someone who was quite unwell would be out of breath and that would also show up in their clinical numbers. With this strain, the numbers will be showing up that they are deteriorating, but they are able to hold a conversation with you and not appear out of breath.”
There is also more chest pain, appetite loss and nausea associated with Omicron, while the ICU are seeing less renal failure requiring dialysis. There is a higher likelihood of single organ failure (most commonly type 1 respiratory) rather than multiple organ failure that they saw with other strains.
Recent genomic analysis of patients in our ICU showed 80% of our COIVD patients had the Omicron variant, with 20% having Delta.