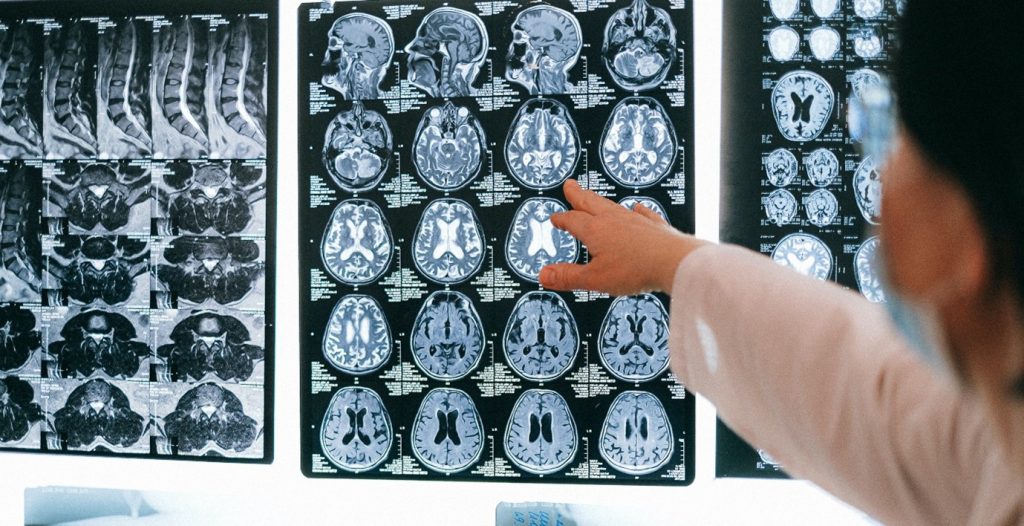
Researchers at the Centre for Cancer Biology have uncovered key evidence to support first in human trials of emerging immunotherapy against deadly brain tumours.
The ground-breaking work has revealed the GD2 molecule on brain cancer cells as a viable target for the exciting chimeric antigen receptor (CAR)-T-cell therapy.
The ‘green light’ for human trials
Glioblastoma multiforme (GBM) is a lethal brain tumour and less than 5 per cent of patients survive longer than five years. This outcome, as well as the desperate need for effective treatments, has changed little in over 30 years.
“These patients have horrible outcomes. They can have surgery, chemotherapy and radiotherapy – and that’s it – and it might buy them six extra months,” said Dr Tessa Gargett, research fellow at the Centre for Cancer Biology, an alliance between CALHN and the University of South Australia.
CAR T-cell therapy: A ‘living drug’
Chimeric antigen receptor CAR-T-cell therapy is an exciting form of immunotherapy that is a standard treatment for some cancers, particularly B-cell leukaemia and lymphoma.
“There are patients who have gone 10 or 15 years with no sign of recurrence following CAR-T cell therapy,” said Dr Gargett.
The personalised therapy involves taking white blood cells from a patient, and re-engineering and replicating their own cancer-killing cells, T-cells, to produce chimeric antigen receptors on their surface. These receptors allow the T-cells to target proteins (antigens) on the surface of cancer cells. Once reinfused in the patient, the cells can recognise and kill the cancer cells.
Choosing the target
One challenge of CAR-T-cell therapy research is knowing which antigen to target.
“Every lab in the field has a specialised capability to target a particular molecule,” said Dr Gargett.
“You need something that’s really high on the tumour and not high in healthy tissue itself to make sure the effect is targeted to the tumour.”
For the Translational Oncology Lab, led by Professor Michael Brown, the target has been a molecule called GD2.
In this landmark study they have successfully confirmed that the GD2 molecule is highly expressed in GBM tissue, making it an ideal target for their GD2-targeted CAR-T-cells.
It’s an essential proof-of-principle before clinical trials can commence.
Importantly, the study also demonstrated that the manufacturing process is viable in this patient group: their blood was healthy enough to provide the white blood cells needed to make the personalised cell therapy.
“This work provides solid evidence to support a human clinical trial,” said Dr Gargett.
Next step: human trials
This work was key to obtaining approval from the Therapeutic Goods Administration (TGA) to commence a first in human trial. A phase 1 clinical trial will open at the Royal Adelaide Hospital in 2023 with Professor Brown as the Principal Investigator. A companion trial for children with diffuse midline glioma will open soon at Sydney Children’s Hospitals Network.
“This laboratory work has laid the ground for us to open trials of CAR-T cell therapy for adult and paediatric patients with aggressive brain cancers to offer these patients the opportunity to participate in clinical studies of new therapies,” said Professor Brown.
According to Dr Gargett, game-changing improvements in cancer treatment options often occur over decades, so researchers don’t always get to witness first-hand the benefits to patients.
“One of the things I appreciate about doing research in CALHN is that you can see an immediate effect of your research in, hopefully, offering something new to patients that wasn’t available before,” said Dr Gargett.
“This is probably the most exciting project I’ve been involved in in my research career.”
This research has been supported by The Hospital Research Foundation, Neurosurgical Research Foundation, and the Health Services Charitable Gifts Board.
Read the research
Click here to read the published paper in the Journal for Immunotherapy of Cancer.